The world of a radiologic technologist is a complex blend of science, technology, and patient care, a field where precision and empathy are equally critical. These healthcare professionals are the unsung heroes of modern medicine, wielding the power of imaging to diagnose and treat a myriad of conditions. From the bustling emergency room to the quiet confines of a specialized clinic, radiologic technologists play an indispensable role in the healthcare ecosystem, providing the crucial visual data that guides physicians’ decisions.
This overview delves into the essential educational pathways, the diverse responsibilities, and the ethical considerations that define the profession. We’ll explore the technological advancements shaping the future of imaging, as well as the career prospects and professional development opportunities available to those who choose this rewarding path. This will provide insights into the crucial skills, knowledge, and ethical standards that are the foundation of this vital role in modern healthcare.
The essential educational pathways leading to a career as a radiologic technologist require thorough exploration.
Radiologic technology offers a dynamic career path within healthcare, requiring a blend of technical expertise and patient care skills. Aspiring radiologic technologists must navigate a structured educational journey to acquire the necessary knowledge and qualifications. This exploration delves into the typical educational requirements, core curriculum, and accreditation processes crucial for entering this field.
Educational Requirements for Radiologic Technologists
Becoming a radiologic technologist necessitates specific educational qualifications, which vary depending on location. These pathways ensure individuals possess the competency to safely and effectively operate imaging equipment and provide patient care.
- Associate’s Degree: This is a common entry point, typically requiring two years of study. Programs cover a broad range of topics, providing a foundational understanding of radiography. Students gain hands-on experience through clinical rotations.
- Bachelor’s Degree: A four-year degree offers a more comprehensive education, often including advanced imaging techniques and management skills. It can lead to leadership roles or specializations. Bachelor’s programs often integrate research components and more extensive clinical practice.
- Certificate Programs: Some hospitals and technical schools offer certificate programs, which may be shorter and more focused on specific areas. These are often suitable for individuals with prior healthcare experience.
Across the United States, most states require licensure, which usually involves completing an accredited program and passing a certification examination administered by the American Registry of Radiologic Technologists (ARRT). The ARRT sets national standards for certification. International requirements differ. In Canada, for instance, certification is managed by the Canadian Association of Medical Radiation Technologists (CAMRT), with accreditation by the Canadian Medical Association (CMA). European countries have varying requirements, often involving national qualifications and professional registration. For example, in the United Kingdom, radiographers typically require a degree in radiography, accredited by the Health and Care Professions Council (HCPC). Australia follows a similar pattern, requiring a degree accredited by the Australian Health Practitioner Regulation Agency (AHPRA). These variations highlight the need for prospective radiologic technologists to research specific requirements based on their desired location of practice. The process ensures a standardized level of competence and safety for patients globally.
Core Curriculum of Radiologic Technology Programs
The curriculum for radiologic technology programs is meticulously designed to equip students with the knowledge and skills required for their profession. The core subjects build a solid foundation in both the theoretical and practical aspects of medical imaging.
The core curriculum commonly includes:
- Anatomy and Physiology: This subject provides a detailed understanding of the human body’s structure and function. Students learn about different body systems, enabling them to visualize and interpret radiographic images effectively.
- Radiation Physics: This is a critical component, covering the principles of radiation production, interaction with matter, and radiation safety. Understanding these principles is essential for minimizing radiation exposure to patients and staff. Students learn about X-ray generation, properties of X-rays, and radiation protection measures.
- Radiographic Positioning: This focuses on the techniques for positioning patients correctly to obtain optimal images. Students learn about various projections, patient preparation, and the use of different imaging equipment.
- Image Evaluation: Students learn to assess the quality of radiographic images, identifying anatomical structures and potential artifacts. They develop critical thinking skills to interpret images and recognize abnormalities.
- Patient Care: This covers essential skills such as patient communication, handling, and safety. Students learn about patient assessment, ethical considerations, and how to provide a supportive environment.
These subjects are typically complemented by clinical rotations, where students apply their knowledge in a real-world setting under the supervision of experienced technologists. This hands-on experience is vital for developing practical skills and patient interaction abilities.
“Radiation physics is the foundation for safe practice, understanding how radiation interacts with the body is paramount.”
Accreditation Bodies and Their Significance
Accreditation plays a vital role in ensuring the quality and standards of education for radiologic technologists. Accreditation bodies evaluate educational programs to ensure they meet specific criteria, thereby preparing graduates for successful careers.
The primary accreditation body in the United States is the Joint Review Committee on Education in Radiologic Technology (JRCERT). JRCERT accreditation signifies that a program meets or exceeds the standards set for radiologic technology education. This accreditation is essential for eligibility to sit for the ARRT certification examination. Programs must undergo periodic reviews and demonstrate ongoing compliance with JRCERT standards.
Other countries have their accreditation processes. In Canada, the CAMRT accredits programs, ensuring alignment with Canadian standards. Accreditation processes involve a comprehensive review of the program’s curriculum, faculty, resources, and clinical facilities. This includes evaluating the program’s effectiveness in achieving its stated goals, the qualifications of its instructors, and the adequacy of its clinical resources.
Graduates from accredited programs are typically better prepared for their careers, as they have received a quality education that meets industry standards. Accreditation also provides assurance to prospective students and employers regarding the quality of the program.
Understanding the diverse responsibilities and duties undertaken by radiologic technologists across various medical settings is crucial.
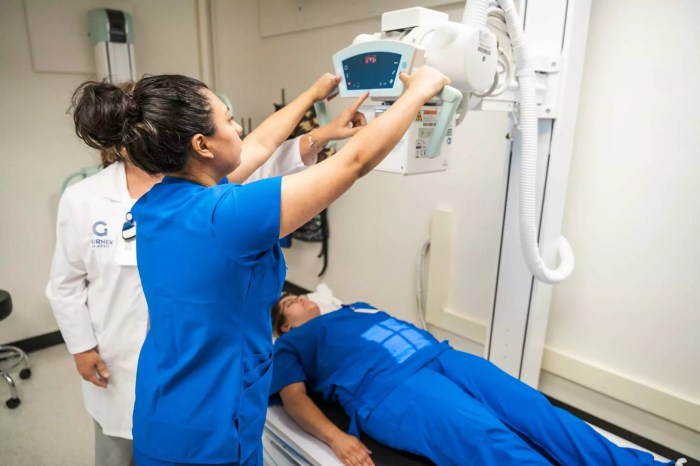
Radiologic technologists are essential healthcare professionals, operating sophisticated imaging equipment to assist physicians in diagnosing and treating medical conditions. Their responsibilities extend far beyond simply pressing buttons; they require a deep understanding of anatomy, physiology, and radiation safety, alongside strong patient care skills. This section explores the breadth of their duties, from the imaging modalities they utilize to the varied environments where they practice.
Imaging Modalities and Applications
Radiologic technologists are proficient in a range of imaging techniques, each with unique applications and requiring specialized knowledge. Their role involves selecting appropriate imaging parameters, ensuring patient safety, and producing high-quality diagnostic images.
X-ray is a fundamental modality, utilizing electromagnetic radiation to visualize bones, the chest, and other internal structures. Technologists position patients, select appropriate exposures, and process the images. It’s often the first line of investigation for suspected fractures, pneumonia, and other conditions.
CT (Computed Tomography) scans use X-rays to create cross-sectional images of the body. Technologists operate the CT scanner, administer contrast agents if needed, and ensure patient comfort throughout the procedure. CT scans are invaluable for detecting tumors, internal bleeding, and other complex medical issues. The technology is rapidly evolving; advancements include reduced radiation doses and improved image resolution, enhancing diagnostic capabilities and patient safety.
MRI (Magnetic Resonance Imaging) employs powerful magnets and radio waves to generate detailed images of organs and tissues without using ionizing radiation. Technologists prepare patients, monitor them during the scan, and operate the MRI equipment. MRI is particularly useful for visualizing the brain, spinal cord, and soft tissues, aiding in the diagnosis of neurological disorders, musculoskeletal injuries, and certain cancers. The technology’s ongoing developments include faster scan times and enhanced image quality, increasing diagnostic accuracy.
Mammography is a specialized form of X-ray imaging used to detect breast cancer. Technologists position patients, compress the breast to obtain clear images, and ensure patient comfort and privacy. Mammography is a critical screening tool for early detection of breast cancer, significantly improving patient outcomes. The introduction of digital mammography and tomosynthesis (3D mammography) has improved image quality and diagnostic accuracy.
Typical Daily Tasks of a Radiologic Technologist
The daily routine of a radiologic technologist is dynamic and patient-centered, encompassing a range of responsibilities that require technical expertise, communication skills, and compassion. Their work is crucial to accurate diagnosis and effective patient care.
Patient preparation is a critical first step. Technologists explain the procedure to the patient, answer their questions, and address any concerns. This may involve positioning the patient correctly, explaining the need for contrast agents, or providing instructions on holding their breath during the scan. Building rapport and ensuring patient comfort are essential for obtaining high-quality images.
Equipment operation is a core responsibility. Technologists operate sophisticated imaging equipment, such as X-ray machines, CT scanners, MRI machines, and mammography units. This involves selecting appropriate imaging parameters, adjusting settings based on patient size and the suspected condition, and ensuring the equipment is functioning correctly. They must also adhere to strict radiation safety protocols to minimize patient and staff exposure.
Image acquisition requires technical skill and attention to detail. Technologists capture images, ensuring they are of sufficient quality for diagnostic purposes. This involves precise positioning of the patient, careful selection of imaging parameters, and meticulous attention to detail. They must be able to recognize and troubleshoot technical issues that may arise during the imaging process.
Patient care is an integral part of the technologist’s role. They monitor patients throughout the procedure, ensuring their comfort and safety. This includes providing emotional support, addressing any anxieties, and monitoring for adverse reactions to contrast agents. They also work closely with physicians and other healthcare professionals to ensure the best possible patient outcomes.
Medical Settings for Radiologic Technologists
Radiologic technologists work in diverse medical environments, each offering unique challenges and rewards. The specific duties and environment vary depending on the setting, but the core responsibility of producing high-quality diagnostic images remains constant.
| Setting | Environment | Typical Procedures | Key Responsibilities |
|---|---|---|---|
| Hospitals | Fast-paced, high-volume environment with a wide range of imaging modalities. | X-rays, CT scans, MRI, fluoroscopy, interventional radiology, and specialized procedures. | Performing a variety of imaging exams, assisting physicians, and managing complex patient cases. |
| Outpatient Clinics | Focused on specific imaging modalities, often with a more scheduled and less urgent workflow. | X-rays, mammography, ultrasound, and potentially CT or MRI. | Performing routine imaging exams, ensuring patient comfort, and managing patient scheduling. |
| Imaging Centers | Dedicated imaging facilities offering a wide range of services, often with advanced technology. | CT scans, MRI, mammography, ultrasound, and other specialized procedures. | Operating advanced imaging equipment, ensuring image quality, and providing excellent patient care. |
| Mobile Imaging Services | Providing imaging services at various locations, such as nursing homes, physician offices, or patient homes. | X-rays, ultrasound, and potentially other modalities. | Traveling to different locations, setting up equipment, and performing imaging exams on-site. |
The vital role of patient care and safety protocols are fundamental aspects of a radiologic technologist’s daily practice.
Radiologic technologists are entrusted with the well-being of patients undergoing diagnostic imaging procedures. Their commitment to patient care and safety protocols is paramount, ensuring the accurate acquisition of images while minimizing potential risks. This responsibility encompasses meticulous adherence to established guidelines, continuous vigilance, and proactive measures to protect patients from unnecessary harm.
Patient Positioning and Shielding Techniques
Proper patient positioning and the strategic use of shielding are critical components of radiation safety. These techniques directly influence the radiation dose a patient receives during an examination, thereby minimizing the potential for long-term health effects.
Effective patient positioning ensures the anatomical area of interest is accurately and completely captured while keeping other areas of the body outside the primary radiation beam. For example, when performing a chest X-ray, the technologist carefully positions the patient upright against the detector, ensuring the shoulders are rotated forward to clear the scapulae from the lung fields. This precise positioning minimizes the need for repeat exposures, which would increase the patient’s radiation dose.
Shielding techniques utilize lead aprons, thyroid shields, and gonadal shields to protect radiosensitive organs from unnecessary exposure. The choice of shielding depends on the specific examination and the patient’s anatomy. Lead aprons, for instance, are commonly used during fluoroscopy procedures to protect the patient’s torso from scattered radiation. Gonadal shielding is frequently employed when imaging the pelvic region, especially in children and individuals of reproductive age. The effectiveness of these shields is based on the principle of attenuation; lead absorbs a significant portion of the radiation, thus reducing the dose to the shielded area.
Furthermore, technologists must be aware of the concept of the “ALARA” principle – “As Low As Reasonably Achievable.” This means minimizing radiation exposure by using the lowest possible radiation dose that still produces a diagnostic-quality image. This involves careful selection of imaging parameters, such as kilovoltage (kVp) and milliampere-seconds (mAs), and the use of collimation to restrict the X-ray beam to the area of interest. Regular equipment maintenance and quality control procedures also contribute to minimizing radiation exposure by ensuring the optimal performance of the imaging equipment.
Protocols for Handling Contrast Media
Contrast media, used to enhance the visibility of anatomical structures during imaging, pose potential risks that necessitate strict adherence to established protocols. These protocols are designed to mitigate adverse reactions and ensure patient safety.
Before administering contrast media, a thorough patient history is essential. The technologist must inquire about any previous allergic reactions to contrast media, pre-existing medical conditions (such as kidney disease, asthma, or diabetes), and current medications. This information helps assess the patient’s risk profile and determine the appropriate contrast agent and administration technique. For example, patients with a history of contrast reactions may require pre-medication with antihistamines or corticosteroids.
During contrast administration, the technologist must closely monitor the patient for any signs of an adverse reaction. These reactions can range from mild (e.g., nausea, itching) to severe (e.g., anaphylaxis, respiratory distress). Immediate access to emergency equipment and medications, such as epinephrine and oxygen, is crucial. The technologist must be trained in recognizing the signs and symptoms of contrast reactions and be prepared to initiate appropriate emergency procedures. This includes notifying the radiologist and the rapid response team.
Furthermore, the technologist must adhere to established guidelines for contrast media preparation, administration, and disposal. This includes verifying the correct contrast agent, dose, and route of administration, as well as ensuring proper aseptic technique to prevent infection. The technologist should also be knowledgeable about the potential risks associated with different types of contrast media, such as the risk of nephrotoxicity (kidney damage) with iodinated contrast agents. For instance, in patients with pre-existing kidney disease, alternative imaging modalities or pre-hydration protocols may be considered to minimize the risk of contrast-induced nephropathy. After the procedure, the technologist provides post-procedure instructions, such as advising the patient to drink plenty of fluids to help eliminate the contrast media from the body.
Essential Patient Communication Skills
Effective communication is crucial for radiologic technologists to build rapport with patients, alleviate anxiety, and ensure a positive imaging experience. The following communication skills are essential:
- Active Listening: Paying close attention to the patient’s concerns, questions, and nonverbal cues. This helps build trust and allows the technologist to understand the patient’s needs and anxieties.
- Clear and Concise Explanation: Providing easy-to-understand explanations of the imaging procedure, including the purpose, process, and any potential sensations the patient may experience. This reduces patient anxiety and promotes cooperation.
- Empathy and Compassion: Demonstrating understanding and concern for the patient’s emotional state. This can involve acknowledging their fears, providing reassurance, and offering words of encouragement.
- Nonverbal Communication: Using positive body language, such as maintaining eye contact, smiling, and using a calm and reassuring tone of voice. This can help create a sense of trust and comfort.
- Cultural Sensitivity: Being aware of and respecting the patient’s cultural background, beliefs, and values. This involves tailoring communication to meet the patient’s individual needs and preferences.
Navigating the legal and ethical considerations in the practice of radiologic technology is a critical responsibility.

Radiologic technologists operate within a complex framework of legal and ethical obligations, ensuring patient safety, maintaining professional integrity, and upholding the standards of the medical profession. These considerations are paramount, shaping every aspect of their practice and demanding a commitment to both legal compliance and ethical conduct. A thorough understanding of these principles is essential for all radiologic technologists.
Ethical Principles Guiding Radiologic Technology
The practice of radiologic technology is guided by a core set of ethical principles that prioritize patient well-being and professional conduct. These principles form the foundation of responsible practice, ensuring that technologists act with integrity and compassion in all interactions. Adherence to these principles is not merely a professional requirement but a moral imperative.
- Patient Confidentiality: Maintaining the privacy of patient information is a cornerstone of ethical practice. Radiologic technologists must protect patient data, refraining from sharing it with unauthorized individuals or entities. This includes safeguarding images, reports, and any other information related to a patient’s medical history. Breaches of confidentiality can have severe consequences, including legal repercussions and damage to the patient-technologist relationship.
- Informed Consent: Obtaining informed consent from patients before any procedure is crucial. This involves providing patients with clear and understandable information about the procedure, including its purpose, potential risks and benefits, and alternative options. Patients must have the opportunity to ask questions and make an informed decision about whether to proceed. This process empowers patients and respects their autonomy.
- Professional Conduct: Radiologic technologists are expected to uphold the highest standards of professional conduct. This includes maintaining competence through continuing education, adhering to professional codes of ethics, and demonstrating respect for patients, colleagues, and other healthcare professionals. Professionalism also encompasses honesty, integrity, and a commitment to lifelong learning.
- Beneficence and Non-Maleficence: Radiologic technologists must act in the best interests of their patients (beneficence) and avoid causing harm (non-maleficence). This involves using the least amount of radiation necessary to obtain a diagnostic image, employing safe practices, and prioritizing patient comfort and well-being. These principles guide decision-making in all aspects of patient care.
- Justice: Ensuring fair and equitable treatment for all patients is essential. This principle requires radiologic technologists to provide the same level of care and attention to all patients, regardless of their background, beliefs, or circumstances. Justice promotes fairness and equal access to healthcare services.
Legal Regulations and Standards for Radiologic Technologists
Radiologic technologists are bound by a range of legal regulations and standards designed to protect patients and ensure the safe and effective use of radiation. These regulations are established by federal, state, and local agencies, and adherence is mandatory. Compliance is not only a professional responsibility but also a legal requirement, with consequences for non-compliance.
- HIPAA Compliance: The Health Insurance Portability and Accountability Act (HIPAA) sets standards for protecting patient health information. Radiologic technologists must comply with HIPAA regulations, safeguarding patient privacy and confidentiality. This includes implementing appropriate security measures to protect electronic health records and other sensitive data. Violations of HIPAA can result in significant penalties.
- Radiation Safety Guidelines: Strict adherence to radiation safety guidelines is essential to protect both patients and technologists from unnecessary radiation exposure. These guidelines include the ALARA principle (As Low As Reasonably Achievable), which emphasizes minimizing radiation dose while obtaining diagnostic images. Technologists must follow established protocols for shielding, collimation, and exposure techniques.
- State and Federal Regulations: Radiologic technologists must comply with state and federal regulations governing the practice of radiologic technology. These regulations may address licensure, certification, continuing education, and other aspects of practice. Technologists are responsible for staying informed about these regulations and ensuring their practice aligns with legal requirements.
- Equipment Standards: The use and maintenance of radiologic equipment are subject to strict standards. Equipment must be regularly inspected and maintained to ensure proper function and safety. Technologists must be trained in the safe operation of all equipment they use and follow established protocols for equipment maintenance and troubleshooting.
- Documentation and Record Keeping: Accurate and complete documentation of all procedures is crucial. Technologists must maintain detailed records of patient examinations, including imaging parameters, patient positioning, and any complications. Proper record-keeping is essential for legal and ethical compliance, as well as for providing continuity of care.
Examples of Ethical Dilemmas in Radiologic Technology
Ethical dilemmas are inherent in healthcare, and radiologic technologists may encounter challenging situations that require careful consideration and ethical decision-making. Addressing these dilemmas involves applying ethical principles, consulting with colleagues, and adhering to institutional policies. The following scenarios illustrate common ethical challenges and how they should be addressed.
- Scenario 1: A patient refuses a necessary imaging procedure due to fear of radiation. Resolution: The technologist should explain the benefits of the procedure, address the patient’s concerns, and provide reassurance. If the patient persists in refusing, the technologist should document the refusal and inform the radiologist or referring physician. The patient’s autonomy must be respected.
- Scenario 2: A technologist discovers a potential error in an imaging study. Resolution: The technologist should immediately inform the radiologist, following established protocols for reporting errors. This may involve repeating the examination or taking additional images to clarify the findings. Transparency and honesty are essential.
- Scenario 3: A colleague is consistently violating radiation safety protocols. Resolution: The technologist should address the issue with the colleague, reminding them of the importance of safety protocols. If the behavior continues, the technologist should report the violation to the supervisor or appropriate authorities, ensuring patient and staff safety.
Exploring the career prospects and professional development opportunities for radiologic technologists is a valuable undertaking.
Radiologic technology offers a dynamic career path with ample opportunities for advancement and specialization. The field’s continued growth, fueled by technological advancements and an aging population, creates a demand for skilled professionals. Understanding the potential for career progression, along with the avenues for specialized training and professional development, is essential for radiologic technologists seeking to maximize their career potential.
Career Progression Paths
The career trajectory for radiologic technologists typically involves a structured progression, often starting with entry-level positions and advancing through experience, education, and certification. This path is often characterized by increasing responsibility and specialization.
- Entry-Level Radiologic Technologist: This is the starting point, focusing on performing general radiographic examinations. Responsibilities include positioning patients, operating radiographic equipment, and ensuring image quality.
- Senior Radiologic Technologist: With experience, technologists may advance to senior positions. They often take on additional responsibilities such as training new staff, supervising daily operations, and contributing to quality control programs.
- Lead Radiologic Technologist: Lead technologists oversee a specific area or modality within a radiology department. They manage staff schedules, ensure compliance with safety protocols, and often act as a liaison between the technologists and the radiology management team.
- Chief Radiologic Technologist/Radiology Manager: This is a leadership role, responsible for the overall management of the radiology department. They handle budgeting, staffing, policy development, and ensuring the department operates efficiently and effectively.
- Specialized Roles: Radiologic technologists can pursue specialized training and certifications in areas such as computed tomography (CT), magnetic resonance imaging (MRI), mammography, and interventional radiology. These specializations often lead to higher salaries and increased career opportunities.
- Education and Research: Some technologists pursue advanced degrees (e.g., Master’s or Doctoral degrees) to work in education, research, or administrative roles within the field.
Specialization Options
Radiologic technologists can specialize in various imaging modalities, each with its unique responsibilities and technical demands. Choosing a specialization often depends on personal interests and career goals.
- Cardiovascular Technology: Cardiovascular technologists assist physicians in diagnosing and treating heart and vascular diseases. They operate specialized equipment to perform procedures like angiograms and cardiac catheterizations. These technologists require a strong understanding of cardiovascular anatomy and physiology, as well as the ability to work in a fast-paced environment. They often work alongside cardiologists and vascular surgeons.
- Nuclear Medicine Technology: Nuclear medicine technologists administer radioactive substances to patients and use specialized imaging equipment (e.g., gamma cameras, PET scanners) to create images that show organ function and detect diseases. This field demands expertise in radiation safety, radiopharmacy, and image interpretation. Nuclear medicine plays a crucial role in diagnosing and staging cancers, as well as evaluating heart and brain function.
- Sonography (Ultrasound): Sonographers use high-frequency sound waves to create images of internal organs and structures. They perform a wide range of examinations, including abdominal, obstetric, and vascular studies. This specialization requires excellent patient communication skills and the ability to interpret complex images. Sonography is non-invasive and provides real-time imaging, making it a valuable diagnostic tool.
Continuing Education and Professional Certifications
Maintaining professional competency and staying current with the latest advancements in radiologic technology requires ongoing education and professional certifications. This commitment to lifelong learning is crucial for career advancement and patient safety.
- Continuing Education (CE) Credits: Radiologic technologists are typically required to earn a specific number of CE credits to maintain their licenses and certifications. These credits can be obtained through various means, including attending conferences, completing online courses, and participating in workshops.
- Advanced Certifications: Technologists can pursue advanced certifications in specific modalities or areas of expertise. Examples include:
- Computed Tomography (CT) Certification: Offered by the American Registry of Radiologic Technologists (ARRT).
- Magnetic Resonance Imaging (MRI) Certification: Also offered by the ARRT.
- Mammography Certification: Requires specific training and ARRT certification.
- Professional Organizations: Joining professional organizations, such as the American Society of Radiologic Technologists (ASRT), provides access to educational resources, networking opportunities, and advocacy efforts.
- Relevant Courses:
- Advanced Imaging Techniques: Courses focusing on the latest advancements in specific imaging modalities.
- Radiation Safety and Protection: Courses that provide up-to-date information on radiation safety protocols and regulations.
- Patient Care and Management: Courses focused on improving patient communication, care, and safety.
- The Importance of Staying Current: Radiologic technology is constantly evolving, with new technologies and techniques emerging regularly. Staying current with these advancements through continuing education ensures technologists provide the highest quality of care and maintain their professional competence.
Understanding the technological advancements that are reshaping the field of radiologic technology offers a modern perspective.
The field of radiologic technology is in a state of constant evolution, driven by rapid advancements in technology. These innovations are not just improving the quality of images but are also transforming the workflows, responsibilities, and overall landscape of the profession. This section delves into the key technological shifts, focusing on digital imaging, emerging modalities, and their impact on the radiologic technologist’s role.
Digital Imaging Technology: Digital Radiography and PACS
Digital imaging has revolutionized radiologic technology, offering significant advantages over traditional film-based methods. Digital radiography (DR) and Picture Archiving and Communication Systems (PACS) are at the forefront of this transformation.
Digital radiography (DR) directly captures X-ray images and converts them into digital data, eliminating the need for film processing. This offers several benefits:
- Reduced Radiation Dose: DR systems often require lower radiation doses to produce high-quality images compared to film-based systems. This directly benefits patient safety.
- Enhanced Image Quality: Digital images can be manipulated and optimized for better visualization of anatomical structures. Features such as windowing and leveling allow for adjustments in brightness and contrast to highlight specific areas of interest.
- Faster Image Acquisition and Availability: Images are available almost instantly, reducing the time patients spend in the imaging room and allowing for quicker diagnoses.
- Improved Workflow Efficiency: Digital images can be easily stored, retrieved, and shared electronically, streamlining the workflow and reducing the physical storage space required.
PACS is a system that manages and stores digital images and associated data. It facilitates the storage, retrieval, distribution, and display of medical images. PACS integrates seamlessly with DR systems, allowing radiologists and other healthcare professionals to access images from anywhere within the network.
- Centralized Image Storage: PACS provides a central repository for all medical images, ensuring easy access and reducing the risk of image loss.
- Remote Access: Authorized users can access images from any location with a network connection, enabling remote consultations and second opinions.
- Image Archiving and Retrieval: PACS allows for efficient archiving and retrieval of images, ensuring that patient records are readily available for future reference.
- Integration with Other Systems: PACS integrates with other healthcare information systems, such as Electronic Health Records (EHRs), providing a comprehensive view of patient data.
The combination of DR and PACS has fundamentally altered the practice of radiologic technology, leading to improved image quality, reduced radiation exposure, enhanced workflow efficiency, and better patient care. The shift to digital imaging represents a significant advancement in the field, enabling more accurate diagnoses and facilitating better patient outcomes.
Final Thoughts

In conclusion, the journey of a radiologic technologist is one of continuous learning and adaptation. From mastering the intricacies of anatomy and radiation physics to embracing cutting-edge imaging technologies, these professionals are at the forefront of medical innovation. As healthcare evolves, the demand for skilled and compassionate radiologic technologists will only increase. Their dedication to patient safety, ethical conduct, and the pursuit of excellence ensures that they will remain integral to the future of healthcare, continuing to illuminate the path to diagnosis and treatment.
